HIE (hypoxic-ischaemic encephalopathy) is a type of brain dysfunction occurring in newborns (neonates) caused by a lack of oxygen (hypoxia) and restricted blood flow (ischaemia) to the brain before, during or shortly after birth[1]. It is a critical, often life-threatening condition and is a leading cause of neonatal mortality and long-term, severe disability, such as cerebral palsy.
HIE can occur in any newborn baby but the term is clinically used in those more mature babies (those born after 34-35 weeks’ gestation). Therapeutic cooling as a treatment is usually limited to those of 37 weeks and above (as these were the babies studied in the TOBY[2] study of therapeutic hypothermia which is the basis for the British Association for Perinatal Medicine guidance on cooling therapy for babies with potential HIE[3]).
In relation to HIE, MNSI is directed to investigate safety events in England, in babies over 37 weeks completed gestation and in whom the mother has been in labour. This means there are a proportion of babies from across the UK managed for HIE that are not reported to or investigated by MNSI.
MNSI reviews babies with a potential severe brain injury diagnosed as occurring in the first seven days of life, when the baby has been:
- Therapeutically cooled (active cooling only), or
- Diagnosed with moderate to severe encephalopathy, consisting of altered state of consciousness (lethargy, stupor or coma) and at least one of the following:
- Hypotonia (decreased muscle tone)
- Abnormal reflexes (linked to the eyes) including oculomotor or pupillary abnormalities
- Absent or weak suck
- Clinical seizures.
Many of these babies will not have a severe brain injury as diagnosed by an MRI scan, and they remain in the potential brain injury group. If there is a confirmed hypoxic injury on the MRI scan, or they have ongoing neurological signs and symptoms, then they are classified as a severe brain injury.
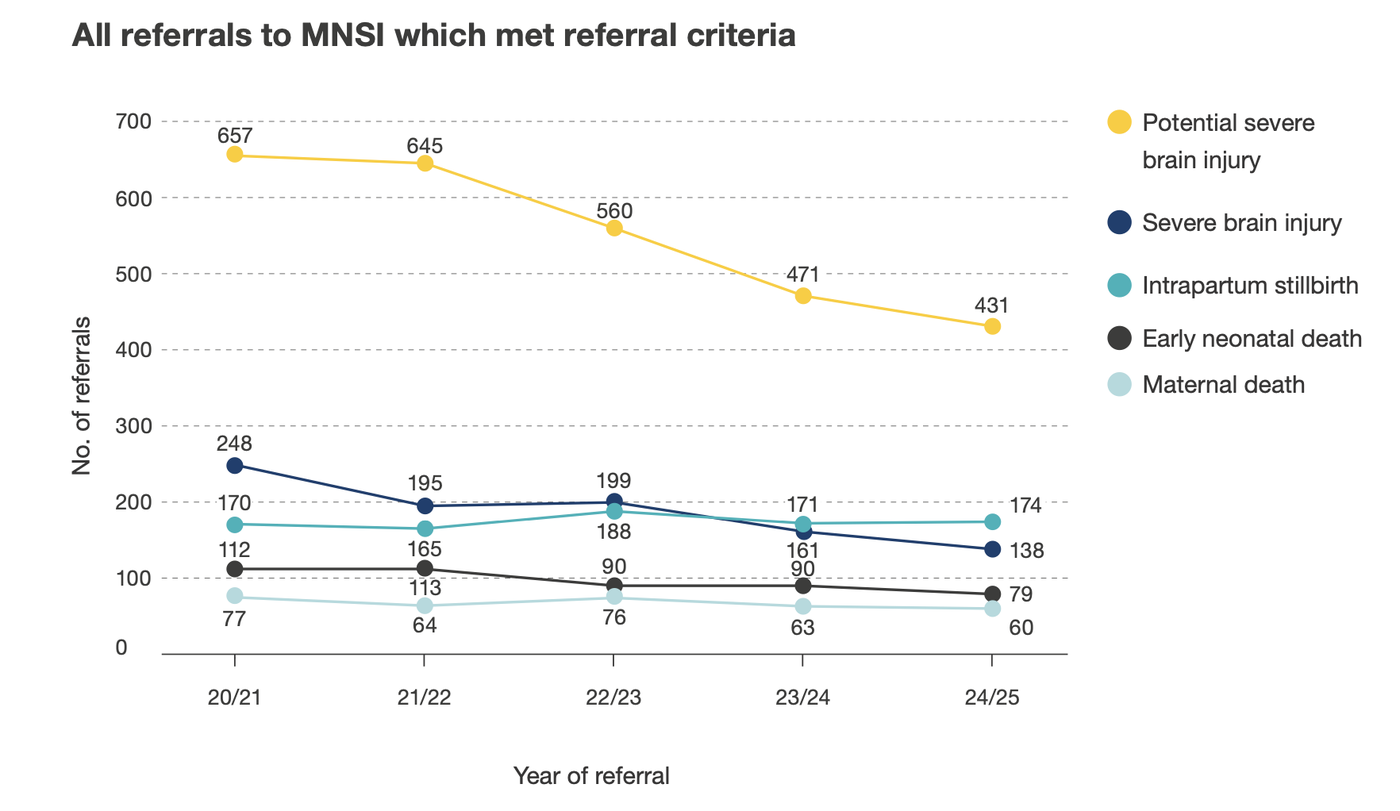
There has been a reduction in the number of babies with a potential severe brain injury reported to MNSI over the last five years (see figure 1). The number of referrals in this category has fallen steadily from 657 babies in 2020/21 to 431 babies in 2024/25. This suggests that there are less term babies being diagnosed with a potential severe brain injury following labour.
There has also been a fall in the number of babies reported to MNSI with a confirmed severe brain injury (as defined by an MRI scan showing hypoxic damage or a baby having ongoing neurological signs or symptoms), from 248 in 2020/21 to 138 in 2024/25.
There has been a fall in the birth rate over these five years and this is likely to have some effect on the total numbers of babies reported. However, the fall in the recorded referral numbers is greater than the fall we might have expected to see in relation to the falling birth rate.
This fall in HIE referrals to MNSI has not been associated with a simultaneous increase in the number of intrapartum stillbirths or early neonatal deaths – these have either remained static or reduced within the MNSI cohort of investigations (as shown in figure 1). A rise in either of these referral groups could have reduced the number of cases of HIE being referred.
As such, it is likely that this represents a reduction in England in the number of babies with HIE, born at term and following labour. The cause of the reduction could have many reasons – one element may be due to improvements in maternity and newborn care supported by the learning shared with NHS Trusts through their work with MNSI (and the predecessor body, the Healthcare Safety Investigation Branch).
[1] As defined by the National Neonatal Research Database (NNRD) in the UK.
[2] https://www.nejm.org/doi/full/10.1056/NEJMoa0900854#tab-contributors
[3] https://www.bapm.org/resources/237-therapeutic-hypothermia-for-neonatal-encephalopathy